The elderly paradox –
when you are older, high blood
cholesterol is a good thing
Conventional
wisdom, which is very influential but almost entirely wrong, tells us that Coronary Heart Disease CHD
is effectively self-induced, by eating the wrong foods in particular. The
diet-cholesterol-heart hypothesis is challenged only by a few, who are
considered to be heretics. In era of preventative medicine, the key to identifying individuals at
particularly high risk of CHD is cholesterol screening.
This
works on the basis that a high serum cholesterol level is an indicator of
cardiovascular death, but the evidence to support this is weak. Like all
population screening exercises, the identification of high cholesterol will
always produce considerable anxiety in the individual; it will always give
someone something else to worry about. Before creating national or even international anxiety (and it
is already too late) it is as well to make certain how useful the
serum cholesterol level of an individual is for predicting the future – we need
to look critically at its predictive value.
The
early work of relating serum cholesterol to future risk was undertaken using
working men as the subjects. However only about 30% of those suffering from a
heart attack fall into this age-group and the majority are above the age of 70
years. Is it reasonable to assume that what is found in middle-aged men is
equally applicable to the elderly?
Doubt
concerning this has been present for some time. We have seen data emerging from
the long-term study of CHD in the town of Framingham, Massachusetts, organised
by the National Heart, Lung, and Blood Institute of the USA. This is a unique study. A publication
recording 30 years of follow-up was entitled “Cholesterol and Mortality” [1].
Its conclusion was quite remarkable and has been followed by what might be
called a stunned silence:
“After
age 50 years there is no increased overall mortality with either high or low
serum cholesterol levels.”
I
use the term stunned silence because this finding has received no publicity and
has no practical impact whatsoever. Remember that about 90% of CHD presents
after the age of 50 years. Think how many people above the age of 50 years have
had their serum cholesterol level tested to try to predict coronary risk when
it doesn’t.
Measuring
the serum cholesterol of middle-aged men cannot be expected to provide any
useful information but it seems to be unstoppable, especially when doctors
receive a financial reward.
The Paris study
The relationship between serum cholesterol and survival has been investigated in a group of 92 women aged 60 years or more who were living in a nursing home in Paris [2]. The women were selected as being free of cancer as it had previously been recognised that serum cholesterol is low in people with cancer. They were followed up for five years and it was quite clear that those with the lowest serum cholesterol had the worst survival.
We can see in Figure 1 that the follow-up of people based on the blood levels of cholesterol. Here we are looking at the death rate. It is high, expressed as deaths per 100 women, as life expectancy is not good in such a group. However it is clear that the death rate is the highest in those with the lowest cholesterol, average 4.5mmol/L. The death rate in those with a serum cholesterol of 4.5mmol/L was five times that of the death rate in those with high cholesterol levels (8mmol/L).
The relationship between death
rate and serum cholesterol turned out to be what is called U-shaped, or J-shaped if
asymmetrical, shown in Figure 2.
The optimum serum cholesterol in this group of women was 7mmol/L, representing those with the lowest mortality rate, standardised as 1. Those women with serum cholesterol greater than 8mmol/L had a slightly higher death rate. However those with lowest serum cholesterol had by far the highest death rate of all. It looks as though a cholesterol level of between 6 and 8 is ideal for women aged 60 or more. This is based on evidence and not dogma.
 |
| Figure 2 - Paris |
The optimum serum cholesterol in this group of women was 7mmol/L, representing those with the lowest mortality rate, standardised as 1. Those women with serum cholesterol greater than 8mmol/L had a slightly higher death rate. However those with lowest serum cholesterol had by far the highest death rate of all. It looks as though a cholesterol level of between 6 and 8 is ideal for women aged 60 or more. This is based on evidence and not dogma.
We can see that the death rate, that is the
risk of dying, increased with increasing age as would be expected. The important
and unexpected fact emerging from the figure is the highest death rate in those
with the lowest serum cholesterol; this is the elderly paradox. The other way to look at the same thing is to record the number or percentage surviving.
The evangelists of the
diet-cholesterol-heart hypothesis might argue that the reason for the high
death rate in those women with low serum cholesterol is that they had or were dying from cancer, but this possibility was eliminated as far as possible at the start of
the study. The authors comment that cancer mortality declines after the age of
70 years, and during the five-year follow-up during which 53 of the 92 women
died, autopsy revealed cancer to be the cause of death in only one.
Another
interesting result, and again paradoxical, is that at the onset of the study
the average serum cholesterol of women known to have CHD was 5.9 mmol/L. In
those who were not known to have CHD, cholesterol was higher at 6.3mmol/L.
The New Haven study
A
further study of the elderly was undertaken in New Haven, Connecticut [3]. This was a community-based study of 997 persons aged more than 70 years with follow-up
for four years. The CHD mortality was once again paradoxical in that a higher
level of serum cholesterol was associated with a lower death rate (Figure 3).
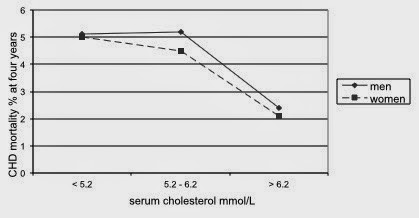 |
| Figure 3 - New Haven - increasing cholesterol, reducing mortality |
The women studied in Paris were in residential care and would have been frail with poor life expectancy (they would have lacked what is called "physiological reserve", not easily measured). Those studied in New Haven were not in supported care and the mortality rate was lower. However the important observation was that those with the lowest cholesterol levels had the highest mortality rates, again five times the mortality rate of those with the highest cholesterol levels. Over the age of 70 it is clearly an advantage to have a blood cholesterol level greater than 6.2mmol/L.
The Honolulu study
The Honolulu study
A
similar result came from the Honolulu Heart Program, a study of 3572 men aged
71 to 93 years[4]. There are two ways of looking at the data. Rather than death rates, the
Figures 4 and 5 show survival over a period of six years in four groups (quartiles)
based on serum cholesterol.
Those with worst survival were those with the lowest cholesterol levels, mean 3.85mmol/L, and this is another example of the elderly paradox. Those with the highest cholesterol level (mean 5.99mom/L) had the best survival.
The results were unchanged when first-year deaths were discounted, the purpose of this being to avoid the possible effect of low serum cholesterol and death being due to undiagnosed cancer.
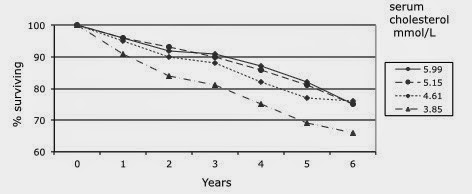 |
| Figure 4 – Honolulu – lowest cholesterol, worst life expectancy |
Those with worst survival were those with the lowest cholesterol levels, mean 3.85mmol/L, and this is another example of the elderly paradox. Those with the highest cholesterol level (mean 5.99mom/L) had the best survival.
 |
| Figure 5 – Honolulu – lowest cholesterol, highest death rate |
The results were unchanged when first-year deaths were discounted, the purpose of this being to avoid the possible effect of low serum cholesterol and death being due to undiagnosed cancer.
Another
interesting observation came out of this study. For the purpose of analysis,
the subjects were divided into two groups, those with risk indicators of CHD
(smoking, hypertension, diabetes or pre-existing manifestations of CHD) and those
without. In both of these groups the mortality rate was lowest in those with
the highest serum cholesterol.
In
those with risk factors, the risk of death for those in highest cholesterol
quartile (mean 5.99) was only 75% the risk of death in those in the lowest quartile (mean 3.85).
If we look at those without risk factors, those in the highest cholesterol
quartile had only 56% risk of death compared to those in the lowest quartile.
Clearly, in this age group above 70 years, low serum cholesterol cannot be
regarded as a good thing.
Why are we not told this?
Why are we not told this?
Conclusion
It
is worth noting some of the statements and conclusions of the authors.
“A
generally held belief is that cholesterol concentrations should be kept low to
lessen the risk of cardiovascular disease. However, studies of the relation
between serum cholesterol and all-cause mortality in elderly people have shown
contrasting results….Only the group with a low cholesterol concentration had a
significant association with mortality…. We have been unable explain our
results. These data cast doubt on the scientific justification for lowering the
cholesterol to very low concentrations in elderly people.”
It
is difficult for medicine and society to absorb the observation that a low
serum cholesterol is associated with a worse health outcome but the evidence is
strong.
The studies also indicate that there is much
more to statin therapy than lowering serum cholesterol. If statins are to be
given then the prescription should not be based on cholesterol measurements.
There is no necessity to measure cholesterol levels in women and in men above
the age of 50 – that is the benefits will not be for those tested, but for the
doctors, the pharmaceutical companies and the academic departments that they
support.
References
1.
Anderson
KM, Castelli WP, Levy D. Cholesterol and mortality: 30 years of follow-up from
the Framingham study. JAMA 1987; 257:
2176-2180.
2.
Forette
B, Tortrat D, Wolmark Y. Cholesterol as risk factor for mortality in elderly
women. Lancet 1989; 333: 868-870.
3.
Krumholtz
HM, Seeman TE, Merrill SS, et al. Lack of association between cholesterol and
coronary heart disease mortality and morbidity and all-cause mortality in
persons older than 70 years. JAMA 1994;
272; 1335-1340.
4.
Schatz
IJ, Masaki K, Yano K, et al. Cholesterol and all-cause mortality in elderly
people from the Honolulu Heart Program: a cohort study. Lancet 2001; 358: 351-355.


You must find all this so frustrating David that the general public just don't accept all this data.
ReplyDeleteI find it frustrating myself!. We have an elderly lady staying with us at the moment - well two years older than me - and she was telling us her doctor had put her on a more modern statin(!) and I think he was trying to bring her down to one of those ridiculously low levels you quote - it was perhaps 5. I think she is 7 at the moment
When I told her about the research you quote she just looks at me as if I was balmy!
I'm late with this question, so perhaps you won't see it, but, here goes. In the research papers do they show the breakdown of the different types of cholesterol? For example, is the drop in total serum cholesterol in older folks due to a drop in HDL levels, or something else?
ReplyDeleteHi Mickey - the studies measured total cholesterol, but this equates to LDL very powerfully. There are attempts to disregard total cholesterol studies with claims that LDL is more "up-to-date" and somehow more powerful. However the widely rested Framingham studies measured total cholesterol. We could call the observations the "Elderly Paradox". There is always the attempt to explain away a paradox such as this that does not fit in with current dogma, but perhaps the paradox is pointing to the truth. The cholesterol story is a house of cards.
DeleteThanks for posting this. I've been collecting information about the effects of myristic acid on cholesterol levels because those 14 carbon chain saturated fatty acid molecules seem to have the greatest impact on total cholesterol as compared to palmitic and lauric acids. Turns out, higher palmitic acid intake is associated with increased muscle mass in chickens. http://www.ncbi.nlm.nih.gov/pubmed/26240391
ReplyDeleteIn hamsters, "increasing amounts of myristic acid (0.03 to 4.2%) do not alter the cholesterol or bile acid metabolism and increase only the HDL-C." https://hal.archives-ouvertes.fr/hal-00900361/document
In Humans, A recent study investigating adipose tissue cell size showed that myristic acid was negatively correlated to BMI and also to cell size (Roberts et al.,2009). While those correlations were for fatty acids in adipose tissue and not in plasma, it does lend some evidence to myristic acid being associated in a health promoting way to body fat. http://www.ncbi.nlm.nih.gov/pubmed/19252892
In the final analysis, it may be that the problem of high serum triglycerides is due to endogenous fatty acid synthesis, not fats found in food. Abstract - "Little is known of the associations of endogenous fatty acids with sudden cardiac arrest (SCA). We investigated the associations of SCA with red blood cell membrane fatty acids that are end products of de novo fatty acid synthesis: myristic acid (14:0), palmitic acid (16:0), palmitoleic acid (16:1 n7), vaccenic acid (18:1 n7), stearic acid (18:0), oleic acid (18:1 n9) and a related fatty acid cis-7 hexadecenoic acid (16:1 n9)...Several fatty acids that are end products of fatty acid synthesis are associated with SCA risk. Further work is needed to investigate if conditions that favor de novo fatty acid synthesis, such as high carbohydrate/low fat diets, might also increase the risk of SCA." http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2882498/