MIT 1, NICE 0
 |
| Massachusetts Institute of Technology |
The results of the randomised controlled trial from Córdoba, Spain, came to attention on September 2nd 2020. It showed a resounding success of the treatment of Covid-19 pneumonia using Calcifediol (25(OH)D), the natural part-activated form of vitamin D.
Córdoba RCT
Controls:
26 patients, standard high quality treatment only.
13 (50%) required transfer to ICU, two died.
Calcifediol treated group:
50 patients, standard high quality treatment + immediate Calcifediol.
1 (2%) required transfer to ICU, no deaths.
This means that compared to the control group, we would have expected 25 (50% of 50) patients in the Calcifediol treatment group to require transfer to ICU, but this was reduced to 1.
24 out of 25 reduction is a 96% reduction, (24/25)x100. This is 96% efficacy.
Response from NICE
I have indicated in a previous post that this study from Córdoba was rubbished by the UK National Institute for Health and Care Excellence (NICE) in a report of September 20th. The commentary was provided by Professor Neil Gittoes, Consultant, Honorary Professor of Endocrinology and Associate Medical Director, University Hospitals Birmingham NHS Foundation Trust; Chair of NHS England specialised endocrinology Clinical Reference Group.
The basis of his report was a series conjectures rather than research.
But it was very effective and the instruction issued to medical staff by NICE was:
"The clinical management of patients with COVID-19 should not be changed based on the results of this study."
This instruction has been followed. It appears that Calcifediol has not been used in the UK. Since September 2nd, more than 16,000 people have died from Covid-19 in the UK, and ICUs are reported as being overwhelmed.
In Switzerland, it has been reported that doctors are recommending that vulnerable people over the age of 60 years, with heart disease or diabetes should sign "Do not Resuscitate" orders so that the ICUs can cope with fewer patients (Times, November 23rd).
Even today the demonstrated benefit of vitamin D as Calcifediol has remained unused.
Analysis by MIT
The world or its medical-scientific advisors appear to going mad, or are seriously negligent. But not the scientists of the Massachusetts Institute of Technology (MIT).
A major analysis of the Córdoba study has been undertaken at the MIT and it came to my attention when I was watching an interview of David Davis MP, one of our very few scientifically trained members of parliament. He has realised the vital importance of vitamin D deficiency in this pandemic and he is struggling to stir the government and the nation into action.
The MIT analysis is one of great detail, and it puts to shame the cursory approach of NICE. It researched the conduct of the study as well as analysing its results.
The conclusion (of MIT analysis) is that there was no fault in the conduct of the Córdoba trial. It acknowledged that the findings (as above) are robust, and that the chance of the results being in error is less than 1 in 60,000.
The paper from MIT contains a lot of statistical maths but the message is stated clearly for those inclined to read it.
Has the MIT report been read by NICE? Is NICE going to respond? Is NICE going to allow medical staff to use Calcifediol in patients seriously ill with Covid-19? Are patients with Covid-19 going to continue to transferred to ICUs in overwhelming numbers? Are people still going to die when they need not?
Is there sufficient Calcifediol
The RCT is being continued in Andalusia, Spain, in a total of five hospitals. Results are due soon and I hear unofficially that Calcifediol has resulted in a 50% reduction of deaths. If the result is so positive there will be no defence in not giving Calcifediol at least to hospital patients with Covid-19 pneumonia. Is there any defence now?
A problem will be the availability of Calcifediol. I hope that the government has the wisdom to obtain large supplies of Calcifediol so as to meet a sudden large demand.
There are several manufacturers of Calcifediol, in China, Korea, India, Netherlands, USA. Most of it used as animal feed, as though we care more about cattle than about humankind.
I can find from a USA website that the cost of Calcifediol is $200 for a 200mcg dose. The dose regimes from Córdoba is 532mcg on admission, 266mcg on days 3, 7, 14 and perhaps 21,28. This appears to be about $200 x 5 = $1,000. In 2003 the cost of one day in an ICU was $1364, likely to be greater now. In the Córdoba RCT the result was a reduction of need for ICU transfer by 96%, a major saving with the cost of Calcifediol being very good value for money.
Sao Paulo, Brazil
An RCT in Brazil investigated giving natural rather than activated vitamin D in an attempt to reduce length of stay of 240 hospital patients admitted with Covid-19 pneumonia.
They were all given standard care but randomly allocated to receive either a single oral dose of vitamin D 200,000 units or a placebo.
The outcome was no difference between the two groups in respect of length of stay, need for ventilation, or death. In those who received the vitamin D supplement the blood level rose, but the the time sequence was not displayed.
What about Vitamin D?
Vitamin D gave no advantage in the Brazil study.
Although this can be regarded as a disappointment to those like me who feel that vitamin D has a great therapeutic potential, perhaps the importance is that of timing.
When we measure the blood level of vitamin D we measure it as its 25-hydroxylated form 25(OH)D, which is Calcifediol. The part-activation process by hydroxylation takes place in the liver, but is rather slow and leisurely. This is fine in general life when are just trying to maintain a steady blood level.
We can see from Figure 1 that for people who are deficient in vitamin D, less than 10ng/ml (25nmol/L), a range of supplement regimens take up to two weeks to increase the blood level above 30ng/ml (75nmol/L, the safe range. Two weeks is much too slow to help a patient who is critically ill with Covid-19 pneumonia, but is adequate for correcting deficiency in a well person.
 |
| Figure 1. Response to vitamin D by mouth, in black is the average of three regimens. In red is 100,000 units per day, in black the average of the regimens. |
There is a distinct pharmaco-kinetic advantage in giving Calcifediol. It bypasses the liver activation process and when given by mouth it will its increase blood to above 30ng/ml (75nmol/L) within about 2 hours. We can see this in Figure 2.
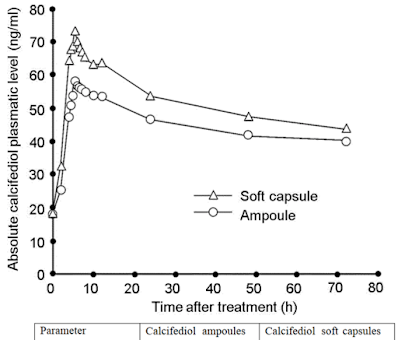 |
| Figure 2. Response to a single dose of Calcifediol |
This means that in a patient admitted to hospital with Covid-19 pneumonia, Calcifediol must be given immediately and natural vitamin D is not an adequate substitute at this stage of emergency.
However natural vitamin D must be given to the well before any illness, and certainly as soon as there is a positive Covid-19 test.


An excellent article as ever and one which clearly explains the link between Vit D and Calcifediol. What is still baffling is the response to this from NICE
ReplyDeleteThank David for the update. I think for too long NICE has disregarded the importance of VItD. However, a re-review has been asked for by Matt Hancock now. I am not sure whether the panellists in NICE would change their minds or not. What concerns me is why haven't our scientists and physicians used the opportunity of the second wave to conduct an appropriate trial using Vit D in different grades of Covid disease??
ReplyDeleteIf your goal is to get 25(OH)D into the blood stream quickly then giving 25(OH)D is the way to go. If your goal is to get 1,25(OH)2D into the VDRs of the immune cells then it MIGHT be quicker to give D3 directly. D3 and 1,25(OH)2D3 can enter immune cells through diffusion but 25(OH)D3 is tightly bound to VDBP and won't enter the cells. D3 can be converted to 1,25(OH)2D3 inside of the cells. The half-life of D3 is around 24 hours so a single 200,000 IU dose won't be as effective as 10,000 given daily. Giving 25(OH)D results in 1,25(OH)2D getting into the cells by being converted by the kidneys and also by macrophages. https://youtu.be/FbheaULwRAk
ReplyDeleteI am not aware that cholecalciferol can enter cells. It would require both 25- and 1- hydroxyls activity. Mu understanding is that only 25(OH)D cane enter cells, and I think the binding to VDBP is not tight and is not inhibiting. I will look it up. A very high dose of oral vitamin D can "switch on" 24-hydroxylase and lead to deactivation of 1,25)OH)D.
DeleteHello Dr.Grimes,
ReplyDeleteexcellent work I really enjoy reading your blog about vitamin D.
The SACN admits that vitamin D supplementation of 400 - 1000 IU has may be an effect on acute respiratory tract infections, but remains on their old recommendations since further RCTs are missing. Concerning a global pandemic, it seems like a joke to me to wait for further RCTs and withhold all the evidence we currently have. A sudden change of their Recommendations and admit that 1000 IU are useful for ARTI is something they try to avoid at all cost.
Dr.Grimes, Would it be possible to use Figure 1. and figure 2. for my own research or is there a link to a study available? Thank You and keep up the good work!
Resource: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/945179/SACN_December2020_VitaminD_AcuteRespiratoryTractInfections.pdf
"The RCT is being continued in Andalusia, Spain, in a total of five hospitals." Do you have links to these RCTs please? I can't find anything. And NICE say there's only these protocols registered NCT04476680; NCT04483635; NCT04386850; NCT04535791. Thanks
ReplyDeleteThe new RCT in Spain is completed, with what I am told are excellent results. Th publication journal has put an embargo on early release of data, but ti should be soon.
DeleteThanks for blog and the books. Would it be possible to post references to the papers or other sources from which the graphs above showing response of 25OHD to D or 25OHD administration.
ReplyDeleteThis is one awesome blog post. Really thank you! same day covid test results
ReplyDelete